How Physical Health Quietly Shapes Your Mental State
Your mindset isn't just in your head. Sleep, gut signaling, and daily habits are quietly running the show — here's the science behind it.
· 11 min read
Key Takeaway
Your Body Is Running Your Mind More Than You Think
Most people treat mental health like a software problem. Therapy, mindset work, journaling, positive reframing — all useful. But the research increasingly points to something most self-improvement content quietly skips: your mental state is also a hardware problem.
Sleep loss, gut dysbiosis, chronic stress, and sedentary routines do not just make you feel physically off. They change the actual biology that produces your emotions, focus, and resilience. The relationship runs in both directions — but for most people living high-output, sleep-deprived, takeout-heavy lives, the body is quietly dragging the mind down first.
According to research on sleep and mental health, gut microbiota and mood disorders, and the microbiota-gut-immune-brain axis, mental state is not separate from physical state. Sleep, gut health, stress biology, and habits quietly shape mood, anxiety, cognition, and resilience — every single day.
Here is what the science actually says, and what you can realistically do about it.
Key Takeaway: Physical health does not just support mental wellbeing indirectly. It shapes it continuously through sleep quality, gut-brain signaling, stress hormones, and the habits you repeat every single day.
Sleep: The Strongest and Cleanest Driver
If you want one lever that touches nearly every aspect of mental health, sleep is it. The research here is unusually clean, and the effect sizes are large enough to matter in real life.
What the Data Actually Shows
A large meta-analysis on sleep quality and mental health found that improving sleep quality led to significant reductions in depression and anxiety symptoms — with additional benefits for rumination and perceived stress. This was not just people feeling more rested. It was measurable psychological improvement driven by a physical intervention.
A separate systematic review and meta-analysis of new shift workers found that both sleep quality and mental health deteriorated after shift work began — and they declined together. That pattern tells you something important: disrupted sleep does not just reflect psychological distress. It can initiate it.
Science Note: A study on acute sleep deprivation and emotion found that even short-term sleep loss increases inflammatory markers, alters cortisol secretion patterns, impairs vigilance, and produces a measurable rise in negative emotional responses. This is not just tiredness — it is a full neuroendocrine disruption event.
Why Sleep Loss Hits So Hard
The mechanism matters here. Sleep deprivation raises systemic inflammation, disrupts the cortisol curve, and degrades real-time emotional regulation. Harvard Health notes that even modest sleep restriction can drive inflammatory pathways associated with mood disorders. Researchers increasingly frame sleep as a transdiagnostic factor — meaning it appears across nearly every mental health condition, not just as a symptom but as a contributing driver.
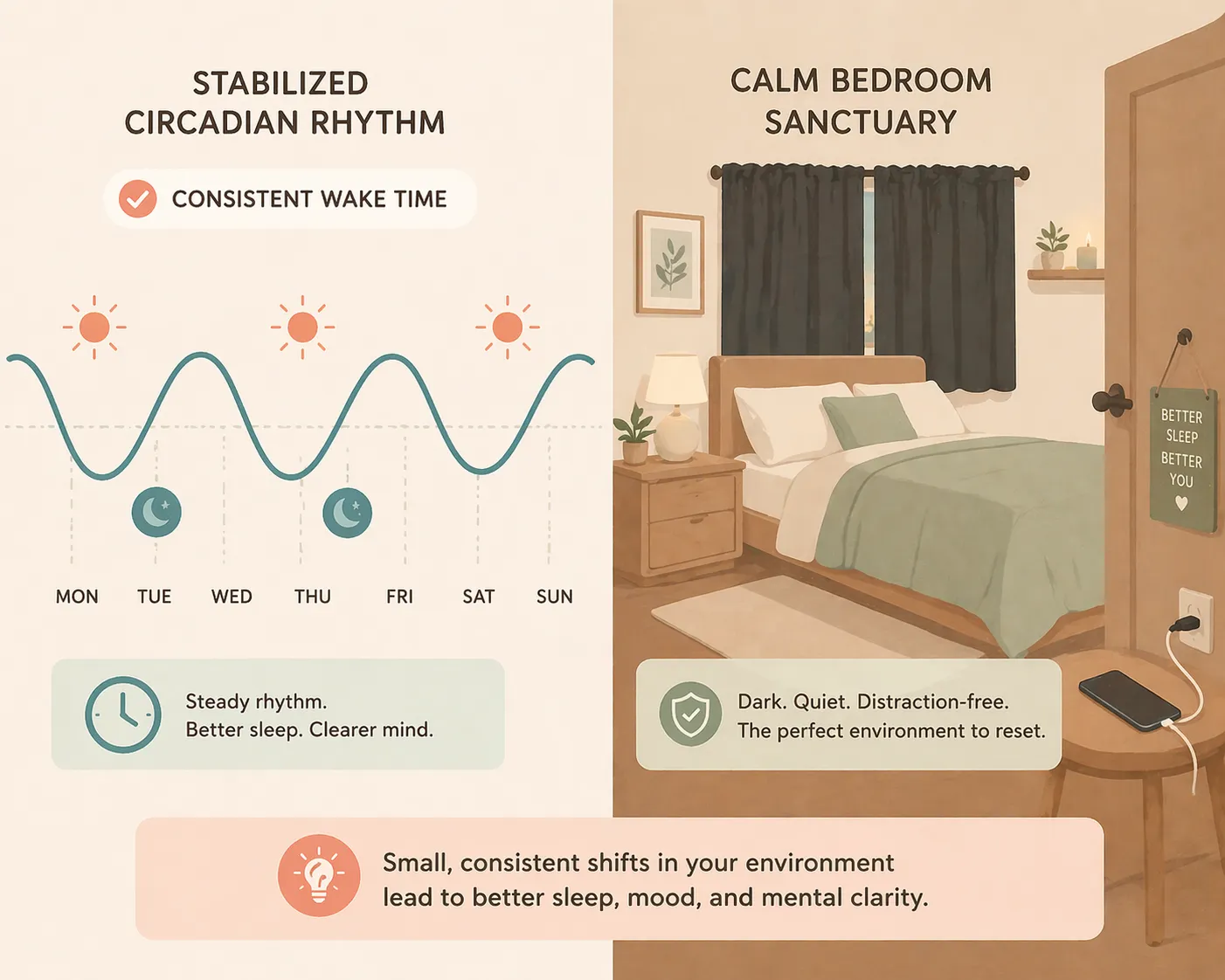
Circadian rhythm deserves its own mention. Irregular sleep timing — not just short duration — destabilizes mood and energy regulation. If you are going to bed at wildly different times each night, your hormonal and stress systems never fully calibrate. You feel it as low motivation, irritability, and that vague sense that something is off, even when nothing in your life has changed.
Vietnam Perspective: Living in Da Nang, the heat alone makes late-night screen scrolling brutal the next morning. Blackout curtains and a small fan cost under 500,000 VND combined and will do more for your sleep — and therefore your mood — than most supplements stacked together. Budget biohacking starts with the boring basics.
What This Means Practically
Prioritize a consistent wake time over total hours if you have to choose one variable to control
Circadian consistency matters as much as duration — irregular timing is its own form of sleep disruption
If your mood has been low for weeks with no obvious cause, ask honestly: how fragmented or inconsistent has your sleep been?
Small environmental changes — light blocking, temperature, phone outside the bedroom — often outperform supplements for sleep quality
The Gut-Brain Axis: The Second Major Pathway
The gut-brain axis has gone from fringe theory to one of the most-cited mechanisms in mental health research. The evidence is still maturing, but the directional findings are consistent enough to take seriously — and the practical implications are accessible even on a tight budget.
How the Gut Talks to the Brain
According to a widely cited review on the gut-brain axis and mood, the gut microbiota communicates with the brain through at least four overlapping channels: neural pathways via the vagus nerve, endocrine signaling, immune modulation, and microbial metabolites. This is not a loose metaphor. These are measurable biological pathways with documented effects on emotional state and stress response.
A healthy microbiome helps maintain intestinal barrier integrity and brain barrier integrity. When dysbiosis occurs — when the balance of microbial species shifts unfavorably — systemic inflammation can increase and cross those barriers, influencing mood, cognition, and stress reactivity from the inside out.
Science Note: Systematic reviews of gut microbiota in anxiety and depression consistently find elevated pro-inflammatory bacterial species and reduced populations of short-chain fatty acid (SCFA) producers. SCFAs help regulate immune function and maintain the gut lining. Their absence is a real physiological gap, not just a missing probiotic label on a supplement shelf.
Gut Health and Emotional Symptoms
A more recent systematic review of gut microbiota variations in depression and anxiety reinforces the pattern: dysbiosis is associated with anxiety and depression across multiple studies, though the human evidence remains mostly correlational rather than fully causal. That distinction matters — it means we cannot yet say definitively that fixing the gut cures depression. But it does mean the gut is a real variable in the equation, not a wellness industry invention.
The most useful clinical reframe is this: when someone reports mood problems with no obvious life-circumstance trigger, gut health is a legitimate variable to investigate — not a replacement for psychological support, but a parallel lane worth addressing.
Try This: For one week, add one fermented food per day. Plain yogurt, kimchi, or natto are all cheap and widely available in Vietnamese supermarkets. You are not curing dysbiosis in a week, but you are starting to shift the microbial inputs your gut receives. Pair it with removing one ultra-processed item you eat automatically, without thinking.
The Bidirectional Loop Between Gut and Sleep
Research also suggests the gut influences sleep quality and emotional regulation in both directions. Gut-derived metabolites, neurotransmitter precursors like serotonin, and circadian-synchronized immune signaling all appear to shape how well you sleep and how emotionally regulated you feel the next day. The gut affects the sleep. The sleep affects the gut. Fix one, and you create conditions for the other to improve.
Stress Biology: The Bridge Between Physical Strain and Emotional Strain
Here is the part most mindset content gets wrong: mindset is real, but it does not operate in a vacuum. It operates inside a body that is either supporting or undermining it constantly.
When the Body Biases Your Thinking
When sleep is poor, inflammation is elevated, or the gut is dysregulated, your brain does not just feel foggy. It shifts toward threat sensitivity, negative interpretation bias, and reduced patience. You become more reactive. Small problems feel larger. Other people become more irritating. Your threshold for frustration drops significantly.
You experience this as a mindset problem — a bad attitude, low motivation, inability to think clearly. But what looks like a cognitive or emotional failure is often partly a physical-state problem. Poor sleep, elevated inflammation, and gut dysregulation can increase irritability, rumination, and threat sensitivity through direct biological mechanisms, not character flaws.
Key Takeaway: Mindset is often downstream of biology, not separate from it. Trying to think your way out of irritability, low mood, or brain fog without addressing the physical inputs is like trying to fix software on a failing hard drive. Sometimes you need to fix the hardware first.
The HPA Axis: Why Stress Is Physical, Not Just Mental
The hypothalamic-pituitary-adrenal (HPA) axis is your body's central stress response system. It coordinates cortisol release, immune modulation, and inflammatory signaling in response to perceived threats — including the low-grade, chronic threats of bad sleep, gut dysbiosis, and constant environmental noise.
According to a detailed review on chronic stress and the microbiota-gut-immune-brain axis, chronic stress links gut, immune, and brain changes together, making physical strain show up as emotional strain. When the HPA axis is chronically activated, the downstream effects include mood dysregulation, poor stress tolerance, and increased anxiety. Physical stressors and psychological stressors use the same biological infrastructure.
Vietnam Perspective: The chronic noise, heat, and traffic of a Vietnamese city is a real HPA axis tax. Most people adapt consciously but not biologically — the stress hormones keep running in the background. Short daily decompression — 10 minutes of genuine quiet, not scrolling — is not a wellness luxury. It is active stress system management on a zero budget.
What Chronic Stress Actually Does to the Body
Sustained HPA activation degrades sleep quality, increases gut permeability, raises baseline inflammation, and shifts immune function in ways that compound over time. This is why people who are chronically stressed often report gut symptoms, poor sleep, and low mood simultaneously — these are not three separate problems. They are three expressions of the same overloaded system.
Chronic stress raises inflammatory cytokines that directly affect mood and cognition
Elevated cortisol over time disrupts sleep architecture, particularly deep and REM sleep
Stress-driven gut permeability allows inflammatory compounds to enter circulation and reach the brain
The immune and nervous systems share signaling molecules, meaning immune activation from any source can shift emotional state
Habits: The Hidden Architecture of Physical and Mental Health
Sleep, gut health, and stress biology do not exist in isolation. They are the output of what you do repeatedly. That is where habits come in — not as a self-improvement concept, but as the daily infrastructure that determines what physical inputs your brain receives, day after day, automatically.

What Habit Research Actually Says
A review on applying habit science to psychological treatments established that habits govern not just exercise and eating patterns but also sleep timing, attentional loops, and even the quality of thinking patterns. Habits are automatic, context-triggered behaviors — and that automaticity is precisely why they are so powerful and so resistant to conscious override.
A systematic review and meta-analysis on health habit formation found that new health behaviors typically take between two and five months to stabilize. Not 21 days, as the popular myth suggests. The average is closer to 59–66 days, with a range that extends significantly beyond that for more complex behaviors. Plan for months. Not weeks.
Science Note: The 21-day habit myth has no empirical basis. The best available meta-analytic data puts average health habit formation at 59–66 days, with a range extending significantly beyond that for complex behaviors. Expecting faster results is one of the most reliable ways to abandon a habit before it has a chance to become automatic.
Why Repeated Inputs Matter More Than One-Time Choices
The insight here is not that one bad night or one greasy meal destroys your mental health. It is that the pattern of inputs — what you eat most nights, when you sleep most nights, how often you move — determines the baseline biological state your brain operates from.
If someone consistently goes to bed late, eats erratically, and stays sedentary, those repeated inputs gradually raise baseline inflammation, drift the circadian rhythm, and erode stress tolerance. Not dramatically or all at once. Quietly, over months, until the person notices their mood has been low with no clear reason and their threshold for stress has shrunk considerably.
Research on physical activity and mental wellbeing and physical activity's role in depression and anxiety consistently shows that regular movement is one of the most reliable physical habits for supporting mental state — not because exercise is magical, but because it reduces baseline inflammation, regulates cortisol, and improves sleep quality, all at once.
Try This: Pick one physical habit that directly feeds a mental health input: a consistent wake time, a 20-minute walk after dinner, or one daily meal built around whole foods. Commit to it for 60 days minimum. Track it with a simple yes or no mark in your notes app each night. You are not optimizing. You are building the infrastructure that everything else runs on.
Habits as Mental Health Infrastructure
The most useful reframe is this: habits are not about discipline or willpower. They are the mechanism by which physical health inputs get delivered — or withheld — on a daily basis. A person with consistent sleep timing, reasonable eating patterns, and regular movement is not just physically healthier. Their brain is receiving consistently better raw material to work with, every single day, without requiring conscious effort.
This also means that mental health support and physical habit change are not competing priorities. They are the same intervention, operating through different entry points. Explore both in parallel on the sleep section and habits section of this site for more targeted breakdowns.
Putting It Together: One System, Not Two
The core insight from all of this research is not complicated, but it is frequently ignored in both wellness culture and clinical practice: physical health and mental health are the same system running in a bidirectional loop.
Sleep loss raises inflammation and worsens mood. Low mood disrupts sleep. Gut dysbiosis promotes anxiety. Anxiety alters gut motility and microbiome composition. Chronic stress degrades sleep, gut integrity, and immune function simultaneously. Bad habits sustain all of it automatically, in the background, without any conscious awareness.
The entry point is wherever you have the most leverage right now. For most people, that is sleep — it has the cleanest evidence and the most immediate downstream effects. Fix the sleep, and gut health, mood stability, and stress tolerance often start to improve without additional intervention. Build one consistent physical habit, and the mental state begins to stabilize without you having to think your way into it.
This is not optimism. It is just how the system works. Start with the hardware, and the software tends to follow.
Science Note
Try This
FAQ
Can improving sleep actually reduce anxiety and depression?
Yes — and this is one of the strongest findings in the physical-mental health research. A large meta-analysis found that interventions targeting sleep quality led to significant reductions in both depression and anxiety symptoms, with additional improvements in rumination and perceived stress. Sleep is not just a symptom of mental health problems — it is an active driver of them. Consistently prioritizing sleep quality and timing is one of the highest-leverage mental health interventions available, and it requires no prescription and no money.
How does gut health affect mood and mental state?
The gut microbiome communicates with the brain through neural pathways — especially the vagus nerve — immune signaling, endocrine hormones, and microbial metabolites. When the microbiome is imbalanced, it tends to increase systemic inflammation and reduce production of short-chain fatty acids, both of which negatively affect brain function and emotional regulation. Systematic reviews consistently find pro-inflammatory microbiome patterns in people with depression and anxiety, though the full causal picture is still being studied.
Why do I feel mentally off even when nothing is wrong in my life?
This is one of the most common and underappreciated experiences in mental health. When sleep is poor, inflammation is elevated, or the gut is dysregulated, your brain shifts toward threat sensitivity and negative interpretation — independent of what is actually happening in your life. You may experience it as low motivation, irritability, or vague anxiety, but the upstream driver can be entirely biological. It is worth auditing sleep quality, eating patterns, and movement before concluding the problem is purely psychological.
How long does it actually take to form a healthy habit?
A systematic review and meta-analysis on health habit formation found that new health behaviors typically take between two and five months to become automatic, with an average of roughly 59 to 66 days. The popular 21-day figure has no solid empirical support. Variation is high — simpler behaviors stabilize faster, complex ones can take considerably longer. The practical takeaway: plan for months, not weeks, and design your environment to support repetition rather than relying on motivation to carry you through.
What is the gut-brain axis and why does it matter for mental health?
The gut-brain axis is the bidirectional communication network between the gastrointestinal tract and the central nervous system. It operates through four main channels: the vagus nerve, immune signaling molecules, hormones, and microbial metabolites. This means your gut bacteria can influence neurotransmitter activity, stress hormone levels, and inflammatory signaling in the brain. It is one of the primary reasons that diet, digestion, and microbiome health have real, measurable effects on mood, anxiety, and cognitive function.
Does chronic stress physically change the body?
Yes. Chronic stress activates the HPA axis — the brain-adrenal system that governs cortisol and inflammatory signaling. When activated persistently, this degrades sleep quality, increases gut permeability, raises baseline inflammation, and shifts immune function in ways that increase anxiety and mood dysregulation. Research frames chronic stress as a key mechanism linking microbiome disruption, immune changes, and poor mental health outcomes together. Stress is not just a feeling — it is a physiological state with measurable systemic consequences.
What is the best first step if I want to improve both physical and mental health at the same time?
Start with sleep consistency. Set a fixed wake time — even on weekends — and protect it for at least four to six weeks. This single variable touches circadian rhythm, cortisol patterns, inflammatory baseline, and emotional regulation simultaneously. It requires no supplements, no equipment, and no expensive program. Once sleep timing is stable, layer in one dietary change targeting gut health and one form of daily movement. Build sequentially rather than all at once, and expect the full compounding effect to emerge over two to three months minimum.
Biohacking without the $10K budget
Get practical weekly insights on sleep, gut health, and mindset, built for real life in Southeast Asia and beyond.
Subscribe freeRelated Articles
The 5-4-3-2-1 Grounding Technique for Anxiety Relief
When anxiety spikes, your brain doesn't need motivation — it needs a circuit breaker. The 5-4-3-2-1 grounding technique is exactly that.
Why You're Still Bloated (Your Gut Microbiome Explains It)
If you're eating clean and still bloated, your gut bacteria are probably the problem — not your diet. Here's what's actually going wrong at the microbial level.
Tired But Can't Sleep? Here's What's Actually Wrong
You're running on empty all day, but the second you lie down, your brain switches on. This isn't a willpower problem — it's a nervous system problem.